Recently, Professor LIU Gang's team, school of Public Health, Huazhong University of Science and Technology, has made new progress in the field of vitamin D and microvascular and macrovascular complications in patients with type 2 diabetes, and the related research results have been published inDiabetes Care and American Journal of Clinical Nutrition.

Evidence is limited regarding the associations between vitamin D status and microvascular complications in individuals with type 2 diabetes (T2D), among whom vitamin D deficiency or insufficiency is particularly common. In this study we aimed to prospectively investigate the associations of serum 25-hydroxyvitamin D [25(OH)D] and vitamin D receptor (VDR) polymorphisms with risk of diabetic microvascular complications.
This analysis included 14,709 participants with T2D who were free of microvascular complications from the UK Biobank. Incidence of diabetic microvascular complications was ascertained via electronic health records. Cox proportional hazards regression models were used to estimate hazard ratios (HRs) and 95% CIs.
Median serum 25(OH)D concentration was 40.7 nmol/L (interquartile range 27.5, 56.4). During a median of 11.2 years of follow-up, 1,370 people developed diabetic microvascular complications. Compared with participants with 25(OH)D <25 nmol/L, individuals with 25(OH)D ≥75 nmol/L had a multivariable-adjusted HR of 0.65 (95% CI 0.51, 0.84) for composite diabetic microvascular complications, 0.62 (0.40, 0.95) for diabetic retinopathy, 0.56 (0.40, 0.79) for diabetic nephropathy, and 0.48 (0.26, 0.89) for diabetic neuropathy. In addition, in comparisons with participants with 25(OH)D <25 nmol/L and minor allele homozygotes (TT of rs1544410 and GG of rs731236), the multivariable-adjusted HRs of composite diabetic microvascular complications were 0.54 (0.38, 0.78) and 0.55 (0.38, 0.80) for participants with serum 25(OH)D ≥50 nmol/L and major allele homozygotes (CC and AA), respectively, although no significant interaction was observed.
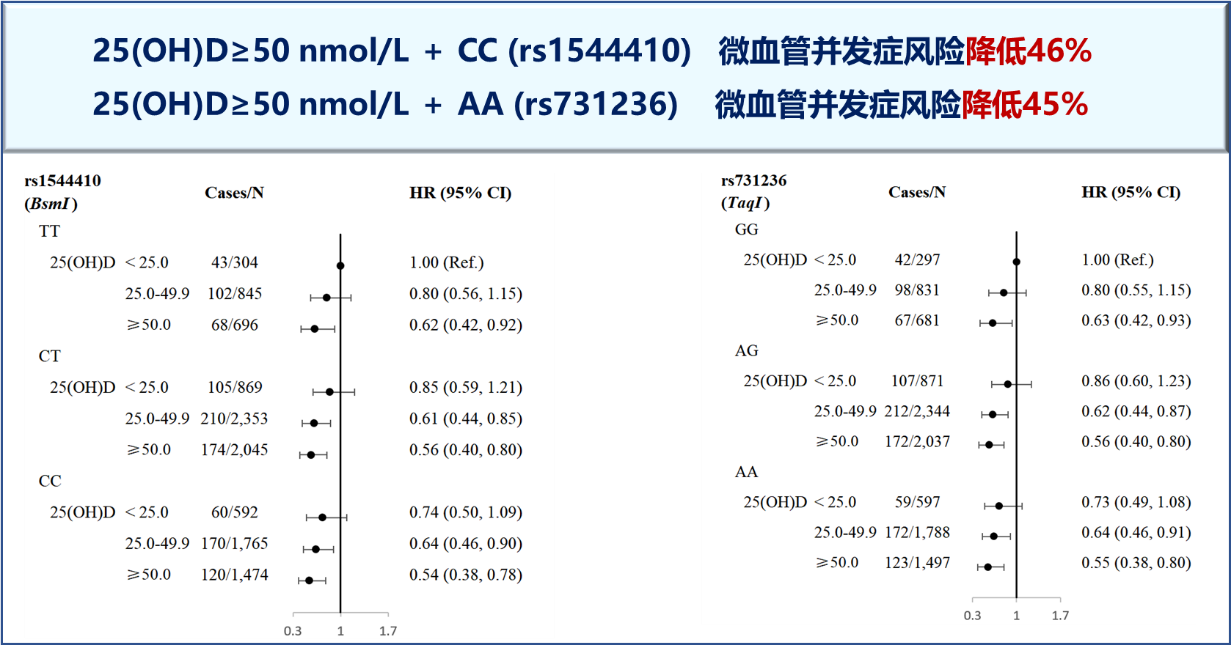
Higher serum 25(OH)D concentrations were significantly associated with lower risk of diabetic microvascular complications, including diabetic retinopathy, diabetic nephropathy, and diabetic neuropathy. Our findings suggest a potential beneficial role of maintaining adequate vitamin D status in the prevention of diabetic microvascular complications.

The presence of a threshold effect has been proposed, suggesting that beneficial effects from vitamin D supplementation may only be present when the vitamin D concentration is below a particular threshold.
We investigated the associations of serum 25-hydroxyvitamin D [25(OH)D] concentrations and genetic factors with risks of total and subtypes of cardiovascular disease (CVD) in individuals with type 2 diabetes (T2D), among whom vitamin D deficiency or insufficiency is particularly common.
This prospective study included 15,103 individuals with T2D who were initially free of CVD and had serum 25(OH)D measurements in the UK Biobank. Incidences of total and subtypes of CVD, including ischemic heart disease (IHD) and stroke, were ascertained via electronic health records. Weighted genetic risk scores (GRSs) were constructed for IHD and stroke.
The mean serum 25(OH)D concentration was 43.4 nmol/L (SD: 20.4 nmol/L), and 65.7% of participants had a vitamin D concentration below 50 nmol/L. During a median of 11.2 years of follow-up, 3534 incident CVD events were documented. Compared with individuals with 25(OH)D concentrations <25 nmol/L, participants with 25(OH)D concentrations ≥75 nmol/L had HRs (95% CIs) of 0.75 (0.64, 0.88) for CVD, 0.69 (0.56, 0.84) for IHD, and 0.74 (0.52, 1.06) for stroke. Participants with 25(OH)D concentrations ≥50 nmol/L and low GRSs, as compared with individuals with 25(OH)D concentrations <25 nmol/L and high GRSs, had a 50% (39%, 65%) lower risk of IHD. No significant interactions were demonstrated between serum 25(OH)D concentrations and the GRSs and genetic variants in vitamin D receptors (VDR).
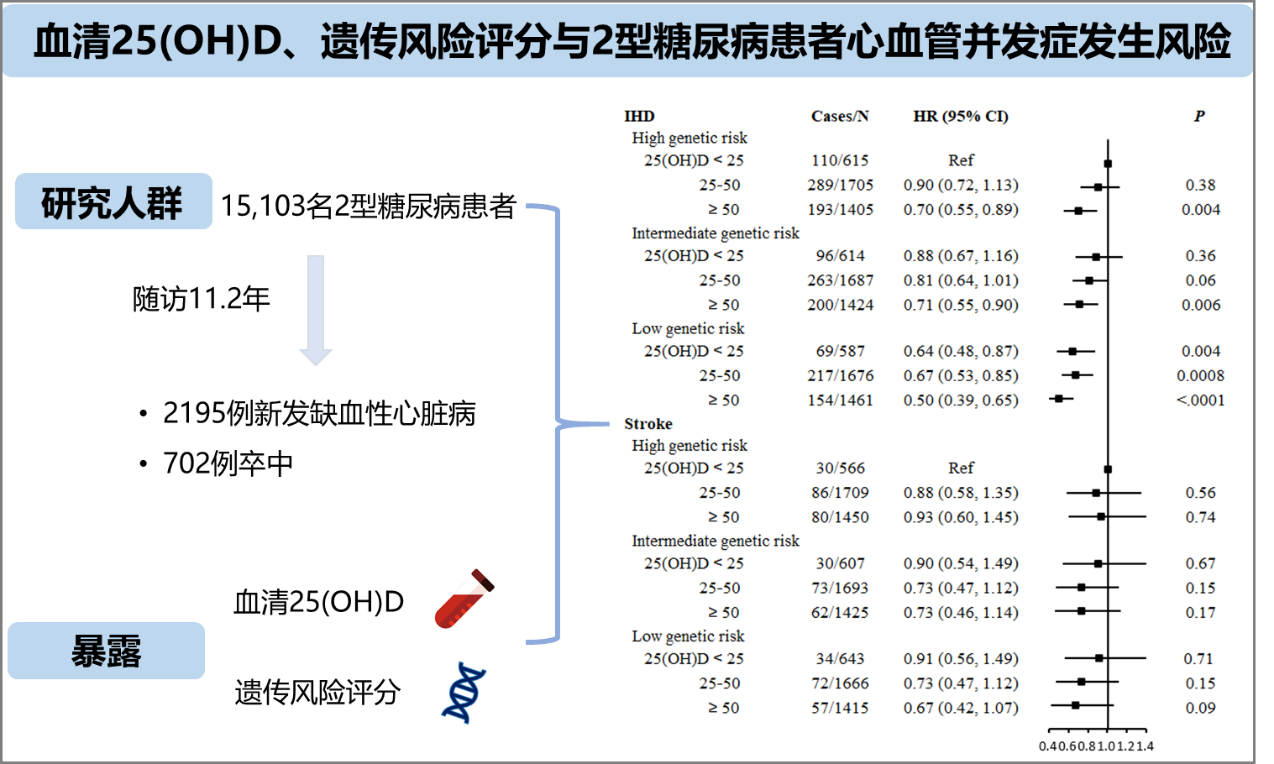
Higher serum 25(OH)D concentrations were significantly associated with lower risks of total CVD and IHD among patients with T2D, regardless of their genetic susceptibility and the genetic variants in VDR. Risk reductions tended to plateau at serum 25(OH)D levels around 50 nmol/L. These findings suggest that maintaining an adequate vitamin D status and avoiding deficiency may help to prevent CVD complications among patients with T2D.
The above studies suggest that vitamin D, as a changeable dietary nutritional factor, may be applied to the prevention of microvascular and macrovascular complications in patients with diabetes. The results of this series of studies provide important population data for vitamin D and health management of patients with type 2 diabetes.
The collaborators of this study include Professor JoAnn E. Manson, member of the National Academy of Medical Sciences, Harvard University, and Professor PAN An, Professor LIU Ligang, Professor SHAN Zhilei, Associate Professor GUO Yanjun and Lecturer CHEN Liangkai, School of Public Health, Huazhong University of Science and Technology. The research is supported by the National Natural Science Foundation of China and the Outstanding Youth Foundation of Hubei Province.
Paper link:
https://doi.org/10.2337/dc22-0513
https://doi.org/10.1093/ajcn/nqac183
